*By the Jase Medical Clinical team* For decades, the dream in oncology has been simple and audacious: teach your own immune system to hunt cancer. Not poison it with chemotherapy. Not burn it with radiation. Train your body's existing defenses to do what they were...
Common Back to School Illnesses
Diligent hygiene is key to preventing most illnesses kids get, but when that’s not enough, medication intervention is common and recommended.

10 Most Common Back to School Illnesses & Physician Recommended Medications
As kids go back to school for the year, most parents expect them to bring home empty lunch boxes, homework, and permission slips, but inevitably they will also bring home an illness. While these illnesses are usually mild, they can often lead to missed school days for your child and missed work days for the caretaker as well as the potential for other people in the family to get sick.
As you prepare new clothes and school supplies for your child, make sure you and your family are also prepared for the sick season as it approaches. Make sure to discuss and emphasize frequent and appropriate hand washing, discourage sharing food/drinks, avoid touching your face, and cover your mouth with a tissue or your elbow if you sneeze or cough, etc. In addition to these basic hygiene measures, consider stocking your medicine cabinet and acquiring a Jase Case* for yourself and your children so you are prepared when illness occurs.
*Always discuss with a medical provider prior to taking any prescription medications. Not all medications listed below are available in all cases and may not be appropriate in all situations.
| Each year about 3 million kids aged 5-17 miss 15 or more school days due to health-related reasons. |
Common Cold
This is one of the most frequent illnesses children get at schools. Colds are caused by different viruses that are easily spread through close-contact environments, like schools and daycares. While there is no cure for the common cold, you can use over-the-counter medications like ibuprofen (Advil), acetaminophen (Tylenol), or cough medications (if age appropriate for your child) to help manage symptoms like fever, body aches, headaches, and cough. Reminder: children should avoid taking Aspirin as it can lead to a rare, but serious condition known as Reye’s disease.
Medications available in the Jase Case: acetaminophen, ibuprofen
Stomach Flu (Gastroenteritis)
The stomach flu (not to be confused with influenza, or flu) is also caused by a virus that can spread rapidly through schools and families. Symptoms of the stomach flu usually include nausea, vomiting, and/or diarrhea. There is also no cure for this illness but symptoms can be managed with rest, fluid and electrolyte replenishment, and over-the-counter and prescription medications depending on symptoms.
Medications available in the Jase Case: loperamide, ondansetron
Strep Throat
Strep throat is caused by a bacteria called Streptococcus pyogenes. Symptoms are usually swollen tonsils, sore throat, swollen lymph nodes, fever, and occasionally abdominal pain. Since this illness is caused by a bacteria, strep needs an antibiotic for treatment after the diagnosis has been confirmed by a medical provider.
Medications available in the Jase Case: amoxicillin, amoxicillin-clavulanate, azithromycin, cephalexin, clindamycin
Influenza (flu)
Influenza, or the “flu”, is caused by a virus that is easily spread in close-contact areas. Common symptoms include fever, chills, body aches, sore throat, cough, and fatigue. There is no cure for this illness, over-the-counter medications like ibuprofen and acetaminophen are often used to help manage symptoms as needed. A prescription medication is also available to help shorten the length of this illness and decrease some complications in high risk individuals.
Medications available in the Jase Case: acetaminophen, ibuprofen, oseltamivir
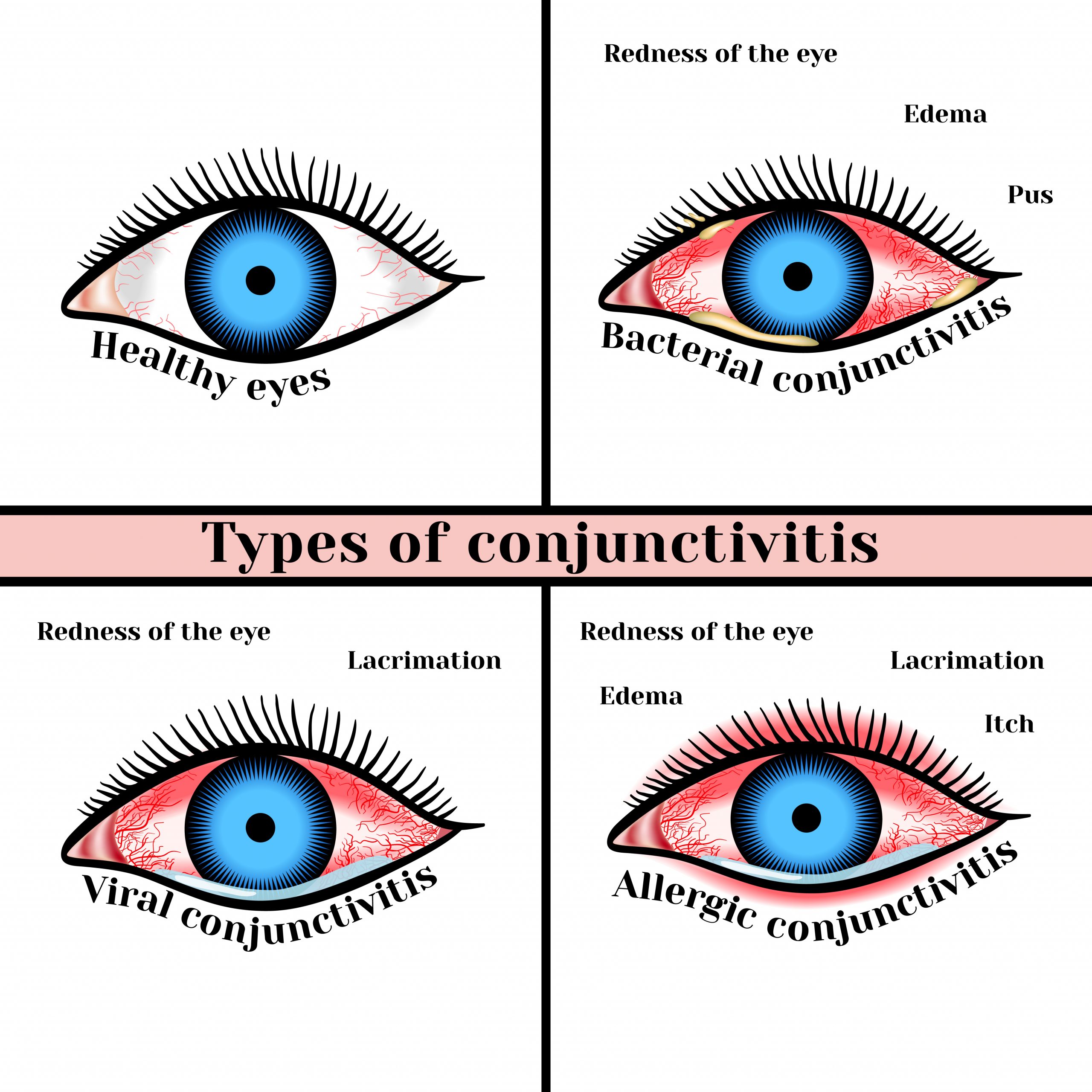
Pink Eye (Conjunctivitis)
Pink eye is a common eye condition that can be caused by either bacteria or virus. Oftentimes symptoms of pink eye are mild and include eye redness, discharge, itchiness, and mild swelling. Despite the cause, this illness is often very contagious and requires missing school or work until symptoms are improved or you have been on medication for at least 24 hours. While it is often difficult to tell the difference between a viral and bacterial cause of this illness, many times an antibiotic eye drop is given.
Medications available in the Jase Case: ofloxacin eye drops
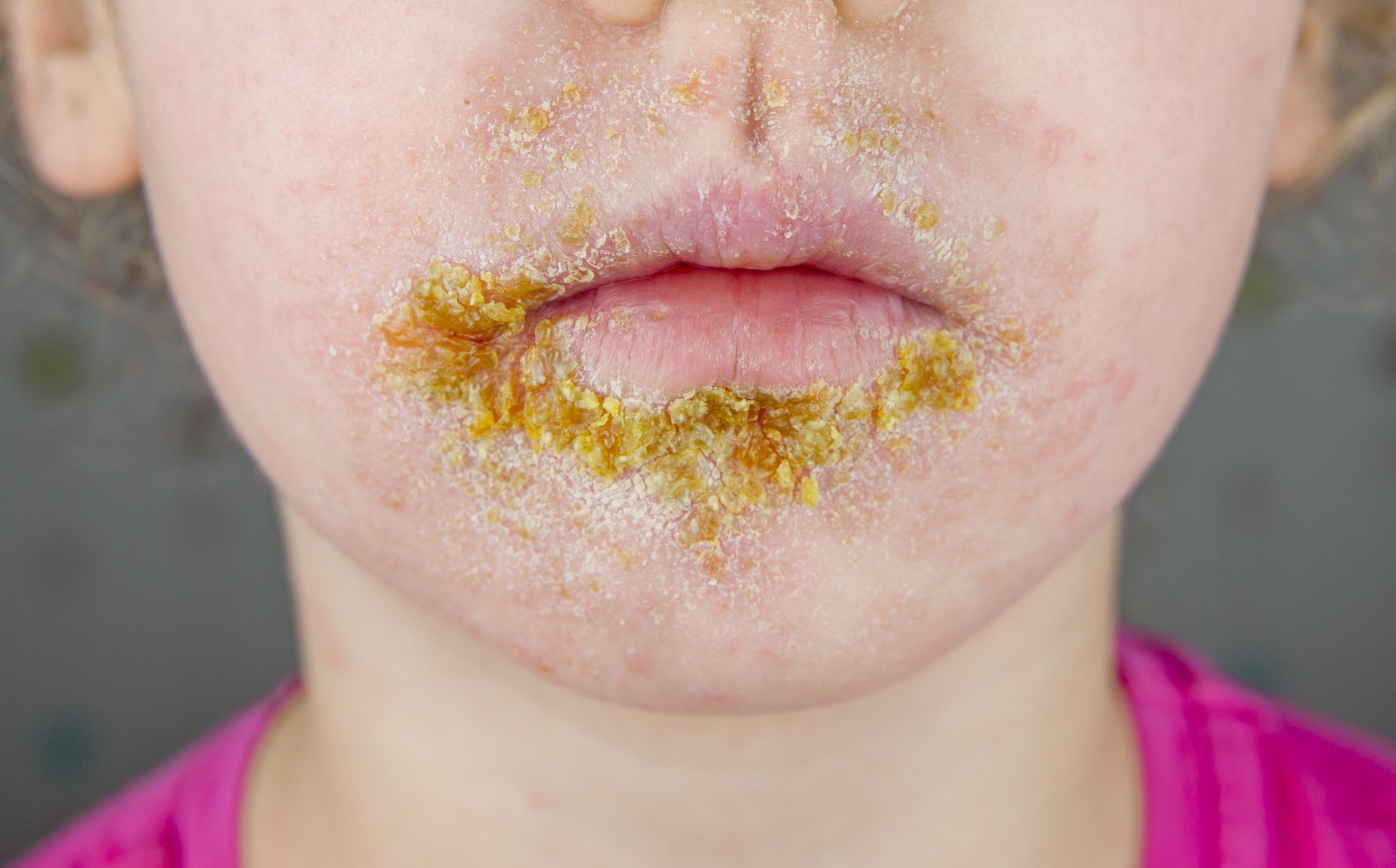
Hand, Foot, Mouth Disease (HFMD)
HFMD is caused by a highly infectious virus and can affect adults and children of all ages, although it is most common in children under 5. This illness causes blister-like sores in and around the mouth and a rash on the hands, feet, and sometimes buttock area in younger children. It is common for the lesions in the mouth to be painful and for a child to refuse eating or drinking due to pain. Most times the lesions on the body are not itchy or painful for the child. While there is no treatment for HFMD, over-the-counter medications and other home remedies (like sucking on popsicles to ease the throat/mouth pain and encourage hydration) can help manage the symptoms.
Medications available in the Jase Case: acetaminophen, ibuprofen
Head Lice
Lice are tiny parasites that live in hair. Although a lice infection is alarming, it is not dangerous. Some people may not experience any symptoms from lice, while others will note excessive scalp itchiness. Adult lice are not always seen on scalp inspection, but the eggs they lay (called nits) attached to hair follicles are always evident in someone who has contracted lice. Treatment for lice includes medicated shampoos that kill lice and manual removal of the nits using a special fine-tooth comb. Oral medication is also available for certain people as well. Clothing, bedding, and soft toys should also be decontaminated to avoid further spread.
Medications available in the Jase Case: ivermectin, permethrin
Chickenpox
Chickenpox, or varicella, is caused by a highly infectious virus. Since the introduction of the varicella vaccination, outbreaks of chickenpox have decreased, but they can still occur. Children who are unvaccinated are at higher risk of infection. Chickenpox causes an itchy, blistery rash but can also have fever, sore throat, headache, fatigue, loss of appetite, and body aches. There is no cure for this illness, but oral and topical over-the-counter medications and creams, as well as other home remedies like oatmeal baths, can be used to help with symptoms or discomfort and itch. Prescription antiviral medications are available to help shorten this illness for adults or other people at high risk of complications but are rarely used in children.
Medications available in the Jase Case: acetaminophen, ibuprofen, loratadine, valacyclovir
Mononucleosis (Mono)
Mononucleosis, also known as “mono” or the “kissing disease”, is caused by the highly contagious Epstein-Barr virus. It is spread by saliva, through kissing, sharing drinks, sneezing, coughing, etc. Symptoms are often similar to flu or strep throat and include fever, sore throat, fever, and muscle aches. There is no treatment for mono, but over-the-counter medications are used to help manage symptoms.
Medications available in the Jase Case: acetaminophen, ibuprofen
Eczema
While eczema is not transmissible between people, it is a common skin condition in many school aged children. Eczema is a type of dermatitis, or skin inflammation, that causes the skin to become itchy, dry, and bumpy. Eczema triggers can vary from person to person, but common triggers include new soaps, detergents, or other chemicals, weather changes, certain fabrics, and stress. While eczema rarely causes school absences, it can be uncomfortable, and is easily treated with avoidance of the trigger and a steroid cream.
Medications in the Jase Case: triamcinolone cream
In conclusion:
Most of us already know that as children return to school, they often bring home more than just homework—they frequently catch and spread illnesses. Despite usually being mild, these conditions can still disrupt family routines and lead to missed school and work days.
To help you combat the illnesses that kids inevitably come home with every school year, we have put together a customized Jase Case containing medications to treat all of the most common back to school illnesses.
Explore the customized Back to School Jase Case HERE
Add all Jase physicians recommended medications to your order and you can customize it further to your exact needs!
As always, stay safe, stay healthy and stay prepared.
– Your partners in preparedness: Jase.com
Lifesaving Medications
Recent Posts
Keeping you informed and safe.
Your Immune System Can Fight Cancer
The 2026 Tick Surge Is Already Here. And It’s Worse Than Doctors Predicted.
*By the Jase Medical Clinical team* I want to tell you something that caught my attention as a physician before it caught my attention as a CEO. A few weeks ago I was reading through case reports from colleagues in the Northeast. Family docs, internists, infectious...
Beyond Chemo: 10 Compounds Researchers Are Studying to Complement Cancer Care
Cancer treatment has always been a moving target. Chemotherapy, radiation, and surgery remain the pillars of oncology — but for decades, researchers have been quietly building a parallel body of literature around compounds that may support, enhance, or complement...
Your Medicine May Be Running Out — And the War in Iran Is Why
Most Americans assume the pharmacy shelf will always be stocked. They assume their blood pressure medication will be there on Tuesday. That ibuprofen will be waiting when they need it. That the cancer drug their spouse depends on won't suddenly be unavailable. That...