The process which the body manufactures, and processes thyroid hormones is very complex. The following is an overview of the thyroid glands anatomy, function, hormones, and nutrients needed for proper function of the thyroid gland. Given this is a very complex gland, take your time reading and going through the video links.
Next post we will delve into thyroid tests and thyroid dysfunction- specifically low and high thyroid.
Thyroid gland and its function
- Anatomy of the thyroid gland
- Function of the thyroid gland
- Hormones produced by the thyroid gland
- Nutrients needed for proper functioning of the thyroid gland
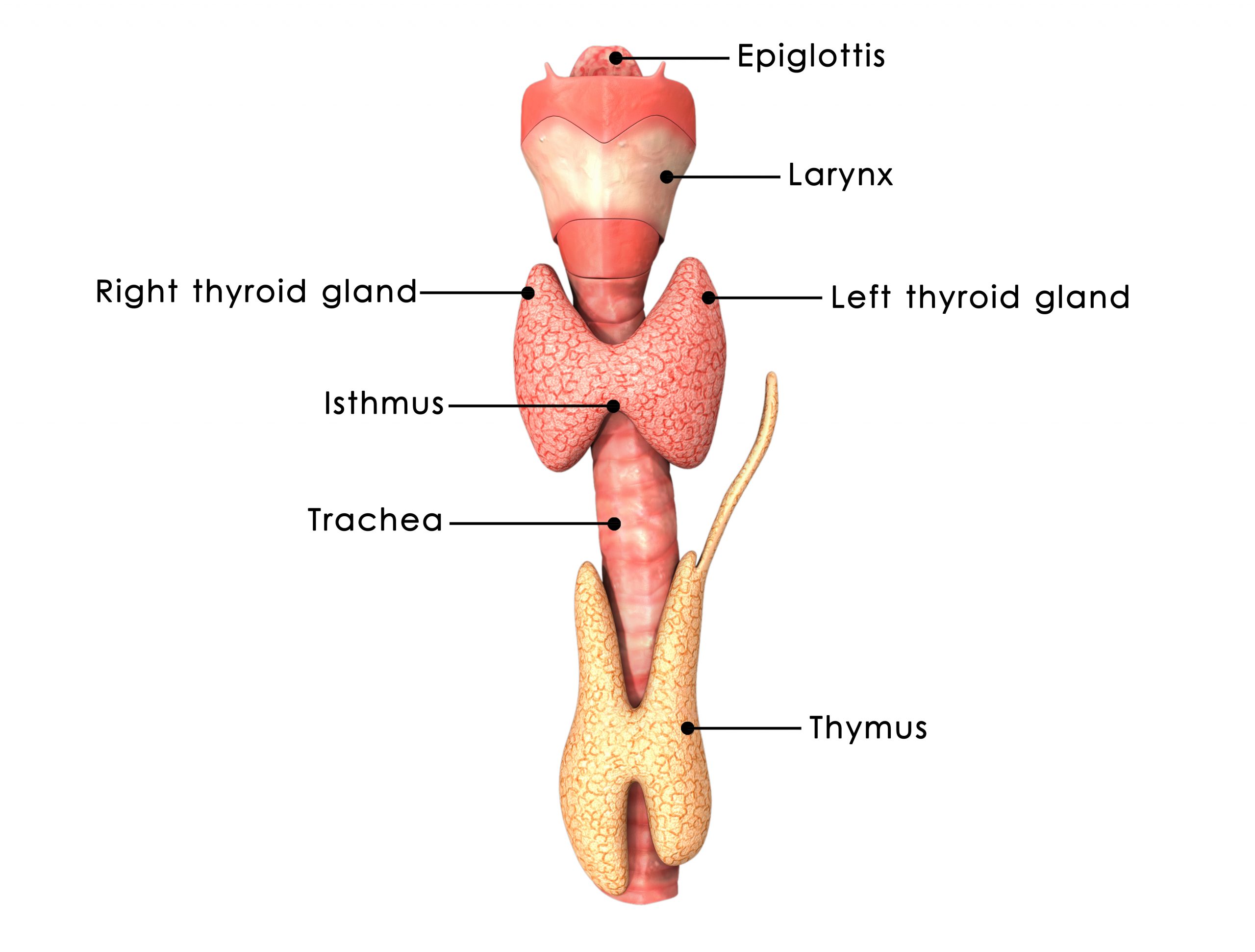
Anatomy of the thyroid gland:
Every cell in the body has thyroid hormone receptors. These receptors control transcription and effect gene expression.
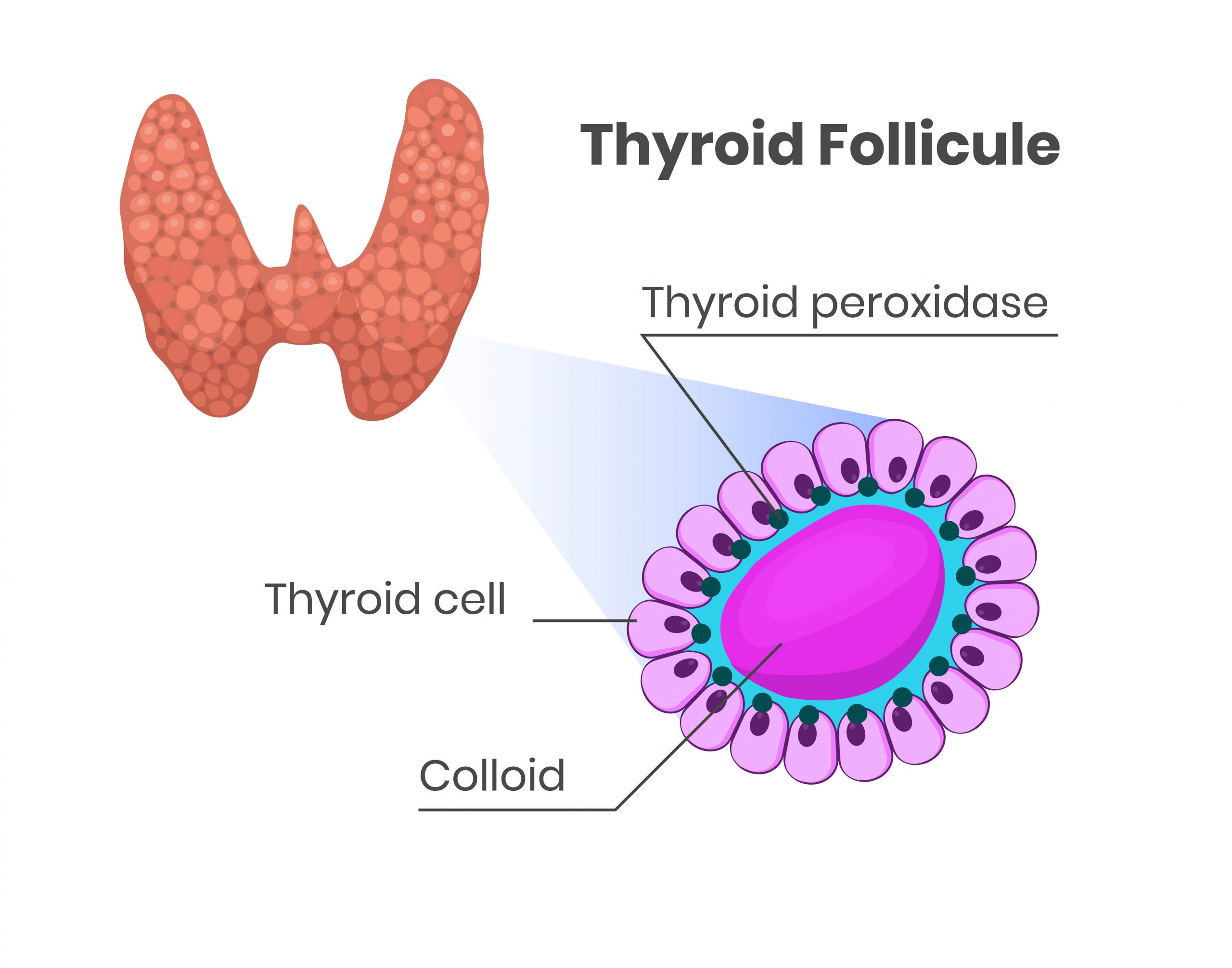
The thyroid gland is one of the largest endocrine glands and consists of two connected lobes. It is found in the neck, below the thyroid cartilage which forms the laryngeal prominence, or “Adam’s apple”. It is a butterfly-shaped organ and is composed of two cone-like lobes or wings, lobus dexter (right lobe) and lobus sinister (left lobe), connected via the isthmus. The thyroid is one of the larger endocrine glands, weighing 2-3 grams in neonates and 18-60 grams in adults, and is increased in pregnancy. The thyroid gland is covered by a thin fibrous sheath, composed of an internal and external layer. The thyroid tissue itself consists of a lot of small individual lobules joined together by thin sheaths of connective tissue. These lobules contain a great number of small vesicles, called follicles, which store thyroid hormones in the form of little droplets. These spherical follicles selectively absorb iodine from the blood for production of thyroid hormones and for storage of iodine in thyroglobulin (a protein present in the thyroid gland, from which thyroid hormones are synthesized). Thyroglobulin is also called colloid. Twenty-five percent of the body’s iodide ions are in the thyroid gland. Inside the follicles, in a region called the follicular lumen, colloid serves as a reservoir of materials for thyroid hormone production and, to a lesser extent, acts as a reservoir for the hormones themselves. The follicles are surrounded by a single layer of thyroid epithelial cells, which secrete T3 and T4. T3, also called triiodothyronine and T4, also called thyroxin are thyroid hormones.
Function of the thyroid gland
The thyroid plays an important role in regulating the body’s metabolism and calcium balance. T4 and T3 hormones stimulate every tissue in the body to produce proteins and increase the amount of oxygen used by cells. The harder the cells work, the harder the organs work. The calcitonin hormone calcitonin works together with the parathyroid hormone to regulate calcium levels in the body. Some of the organ systems thyroid hormones regulate are:
- Respiratory system– regulation of respiratory rate and ventilatory response to hypercapnia and hypoxia
- Renal (kidney)– glomerular filtration rate and blood flow to the kidneys
- Cardiovascular– regulates heart rate, force of cardiac contractions, stroke volume, cardiac output, catecholamine receptors
- Metabolism- regulates glucose absorption in the gastrointestinal track, regulates insulin receptors
- Growth and tissue development– regulates growth and maturation of bones and teeth, also regulates growth and maturation of epidermis, hair follicles and nails. Regulates force and rate of skeletal muscle contractions.
- Nervous system-thyroid hormones are critical for neuronal development, Enhances memory and alertness.
Hormones produced by the thyroid gland
Check out this video on thyroid gland synthesis
What are the thyroid hormones and what substances do they contain? The thyroid hormones T3 (triiodothyronine) and T4 (thyroxine) are made of an amino acid, tyrosine, and an iodine molecule. For the hormone to be synthesized it must complete the following steps:
- Tyrosine, an amino acid that is provided by thyroid epithelial cells and secreted into the lumen of the follicle by a large glycoprotein scaffold called thyroglobulin. Thyroglobulin, as noted above is also called colloid.
- Iodine (or more accurately iodide) is taken up from blood by
thyroid epithelial cells which has an outer plasma membrane called a sodium-iodide symporter, or more commonly known as an “iodine trap”. Once inside the cell, iodide is transported into the lumen of the follicle along with thyroglobulin.
3. The thyroid hormone requires an enzyme called thyroid peroxidase to join the tyrosine with the iodine. The tyrosine will receive either one or two iodine. The term T1 represents one tyrosine and one iodine molecule. T2 represents one tyrosine and two iodine molecules.
4. These, meaning T1 and T2, further combine through the enzyme thyroid peroxidase (TPO) to make the final thyroid hormones: T1+T2=T3 and T2+T2=T4. The byproduct from both reactions is hydrogen peroxide.
5. The thyroid hormone is bound to thyroglobulin and is liberated by hydrolytic enzymes that digest thyroglobulin.
6. The thyroid hormone diffuses out of the lysosomes and into the blood where they bind to carrier proteins and are transported to target cells in the body.
In other words,
T1+T2=T3+ hydrogen peroxide, and
T2+T2=T4+ hydrogen peroxide
Note:
T3 is up to four times more biologically active than T4. Only twenty percent of the body’s T3 is made by the combination of the T1 and T2 molecules. The additional eighty percent is made by T4 losing an iodine molecule in a process carried out in the organs such as the liver.
How is thyroid hormone regulated?
Hormonal output from the thyroid is regulated by thyroid-stimulating hormone (TSH) produced by the anterior pituitary, which itself is regulated by thyrotropin-releasing hormone (TRH) produced by the hypothalamus in a negative feedback loop.
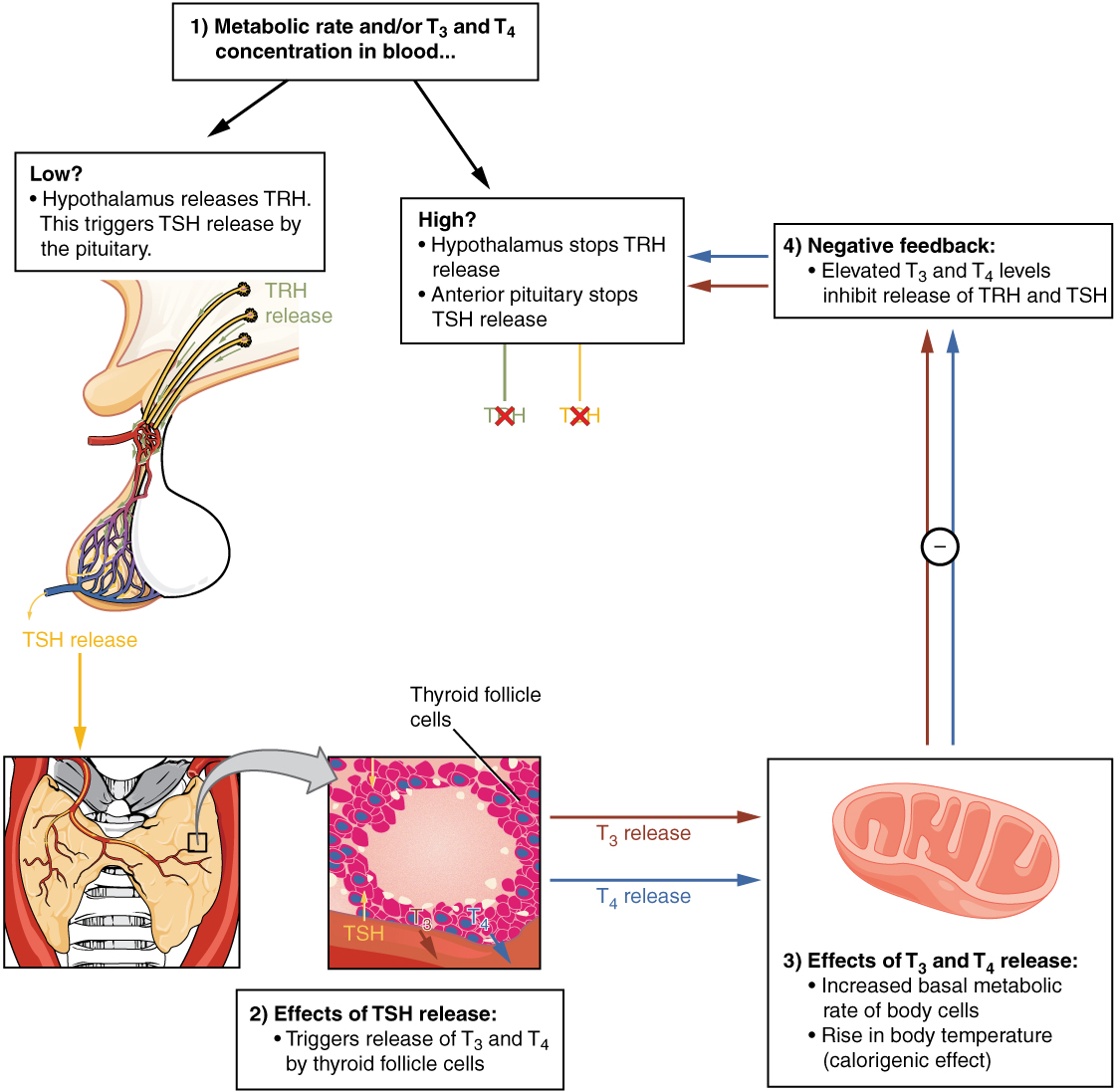
This is described as follows:
HYPOTHALMUS-Signaled by low thyroid hormones the hypothalamus releases TRH (thyrotropin releasing hormone) which stimulates the pituitary gland, *Illustration depicts both high and low thyroid hormone events.
ANTERIOR PITUITARY GLAND– Releases TSH (thyroid stimulating hormone) into the bloodstream, which reaches the thyroid gland
THYROID GLAND –TSH (Thyroid stimulating hormone) causes thyroid gland to release thyroid hormones (T4 and T3 )
When enough T4 and T3 are in the bloodstream it signals the hypothalamus to stop releasing TRH (thyrotropin releasing hormone)
Nutrients needed by the thyroid gland
For the thyroid gland to function properly it requires a supply of nutrients
Selenium– Selenium content in the thyroid is higher than any part of the body. It is a naturally occurring trace mineral found in our foods and soil. One of the challenges with obtaining selenium from our food sources is that the levels can vary dramatically. Brazil nuts are known to be a rich source of selenium, but their selenium content varies according to the region they are grown in.
Selenium is converted into three types of selenoproteins or seleno-enzymes, both terms are interchangeable. The three types of selenoproteins are:
- GPx (glutathione peroxidase) are antioxidants and best known of the selenoproteins
- TRx- (thioredoxin reductases) are involved in cell growth and structure
- Dis (iodothyronine deiodinases) are involved in the conversion of T4 to T3 and other metabolic functions.
A selenium deficiency along with an iodine deficiency is implicated in goiters.
Iodine- Iodine is an essential element that is also needed from our environment. It is one of the building blocks of the thyroid molecule. For the body to be able to utilize iodine, it must be converted to iodide. This is accomplished through the thyroid peroxidase (TPO) reaction. Once this occurs, the free iodine joins with tyrosine to make the thyroid molecule, with hydrogen peroxide as the byproduct.
The group of molecules called the halogens; fluorine, bromine and chlorine mimic iodine and attach to tyrosine thereby rendering the tyrosine molecule useless. This means that your body is not getting the T4 or T3 it needs. Sources of iodine include kelp, sea vegetables, cow’s milk, eggs, tuna, and navy beans. There are several over the counter iodine supplements. Caution should be exercised when using supplemental iodine. When there is an excess of iodine along with a deficiency of selenium, an autoimmune condition called Hashimotos thyroiditis may occur.
Tyrosine– Tyrosine is a nonessential amino acid the body makes from another amino acid called phenylalanine. It combines with iodine to form thyroid hormones. Tyrosine is also the precursor to neurotransmitters dopamine, epinephrine and norepinephrine. It is rare to have a deficiency in tyrosine and supplements are usually not recommended. Dietary sources of tyrosine are chicken, turkey, fish, peanuts, almonds, avocados, bananas, milk, cheese, yogurt, cottage cheese, lima beans, pumpkin seeds, and sesame seeds.
Zinc– Zinc is required to transform the inactive thyroid hormone T4 into the active form T3. It plays an important role in immune function, wound healing, blood clotting, reproduction, growth and smell. Zinc supplementation should be approached carefully. If too much zinc is taken, a copper and iron deficiency can result. Also, taking too much zinc intake can contribute to hyperthyroidism and copper deficiency. Foods rich in zinc are raw pumpkin seeds, oysters, wheat germ, and lamb.
Iron (Ferritin) – Iron requires a high stomach acid for transport into the cells. Many people take iron tablets, and their iron levels stay the same due to low stomach acid. Having low iron levels decreases deiodinase activity. It slows down the conversion of T4 to T3. Insufficient iron levels may affect thyroid hormone synthesis by reducing the activity of the enzyme thyroid peroxidase (TPO) which is dependent on iron. Thyroid peroxidase (TPO) brings about the chemical reactions of adding iodine to tyrosine (amino acid), which then produces T4 and T3. Insufficient iron levels alter and reduce the conversion of T4 to T3. Low iron levels can also increase circulating concentrations of TSH (thyroid stimulating hormone).
Apple cider vinegar or Betaine, a supplement which enhances stomach acidity, promotes protein breakdown and iron absorption. The most bioavailable form of iron is called heme and is found in liver and meats.
- Brooke Lounsbury
Medical Content Writer
Lifesaving Medications
Recent Posts
Keeping you informed and safe.
The War Nobody Prepared For: How the Iran Conflict Is Threatening Your Medicine Cabinet
*By the Jase Medical Clinical team* Most Americans think of war as something that happens somewhere else, visible mainly through a screen. The Iran conflict has found its way into something far more intimate: the medicine bottles in your bathroom cabinet.Since Iran...
Your Immune System Can Fight Cancer
*By the Jase Medical Clinical team* For decades, the dream in oncology has been simple and audacious: teach your own immune system to hunt cancer. Not poison it with chemotherapy. Not burn it with radiation. Train your body's existing defenses to do what they were...
The 2026 Tick Surge Is Already Here. And It’s Worse Than Doctors Predicted.
*By the Jase Medical Clinical team* I want to tell you something that caught my attention as a physician before it caught my attention as a CEO. A few weeks ago I was reading through case reports from colleagues in the Northeast. Family docs, internists, infectious...