(This is part 1 of a series on diabetes, other parts will delve into labs, testing, prevention and management of diabetes)
A recent study revealed that Thai farmers exposed to different pesticides found an association between 3 different pesticides and onset of type 2 diabetes.
According to the study, a population-based case-controlled study was conducted among residents in the Bang Rakam district of Phitsanulok Province in Thailand. Lifetime pesticide exposure and other relevant data were collected from 866 participating cases with diabetes mellitus and 1021 healthy controls. Among 35 individual brand-named pesticides investigated, they found statistically significant occurrences of type 2 diabetes with three insecticides.
3 Pesticides
A popular insecticide, trade name Sevin, (carbaryl) recently banned for homeowner use but still available for commercial application was found to have a casual association to the onset of type 2 diabetes, along with other health issues. This insecticide was pulled from consumer shelves mid 2020 but is still used on industrial crops. Another insecticide, mevinphos has been on the EPA restricted use list, but is banned in the EU, and endosulfin whiles still being used on U.S. crops is being phased out globally.
In addition, another popular pesticide, Roundup (glyphosate) may also contribute to type 2 diabetes according to a 2022 study titled “Impact of Glyphosate on the Development of Insulin Resistance in Experimental Diabetic Rats: Role of NFκB Signalling Pathways”.
What is diabetes?
Diabetes is a chronic, serious health issue facing over 10 percent of the U.S. population, and one in five people with diabetes don’t even know they have it. It is a leading cause of death due to complications, such as heart disease, stroke, blindness, kidney failure and lower limb amputation. Depending on the type of diabetes, insulin and glucose metabolism are involved. While the link between pesticide use is a contributing factor, many other life choices and genetics play into the development of diabetes.
All diabetes is diagnosed through bloodwork, by checking glucose readings- either fasting, after meals or both. A urine dip can show high glucose levels, indicating the need for further testing via bloodwork.
Types of Diabetes
Prediabetes is a serious health condition where blood sugar levels are higher than normal, but not high enough yet to be diagnosed as type 2 diabetes. Approximately 96 million American adults—more than 1 in 3—have prediabetes. Of those with prediabetes, more than 80% don’t know they have it. Prediabetes puts you at increased risk of developing type 2 diabetes, heart disease, and stroke.
Insulin is key factor
Insulin is a hormone made by your pancreas that acts like a key to let blood sugar into cells for use as energy. If you have prediabetes, the cells in your body don’t respond normally to insulin. Your pancreas makes more insulin to try to get cells to respond. Eventually your pancreas can’t keep up, and your blood sugar rises, setting the stage for prediabetes—and type 2 diabetes down the road.
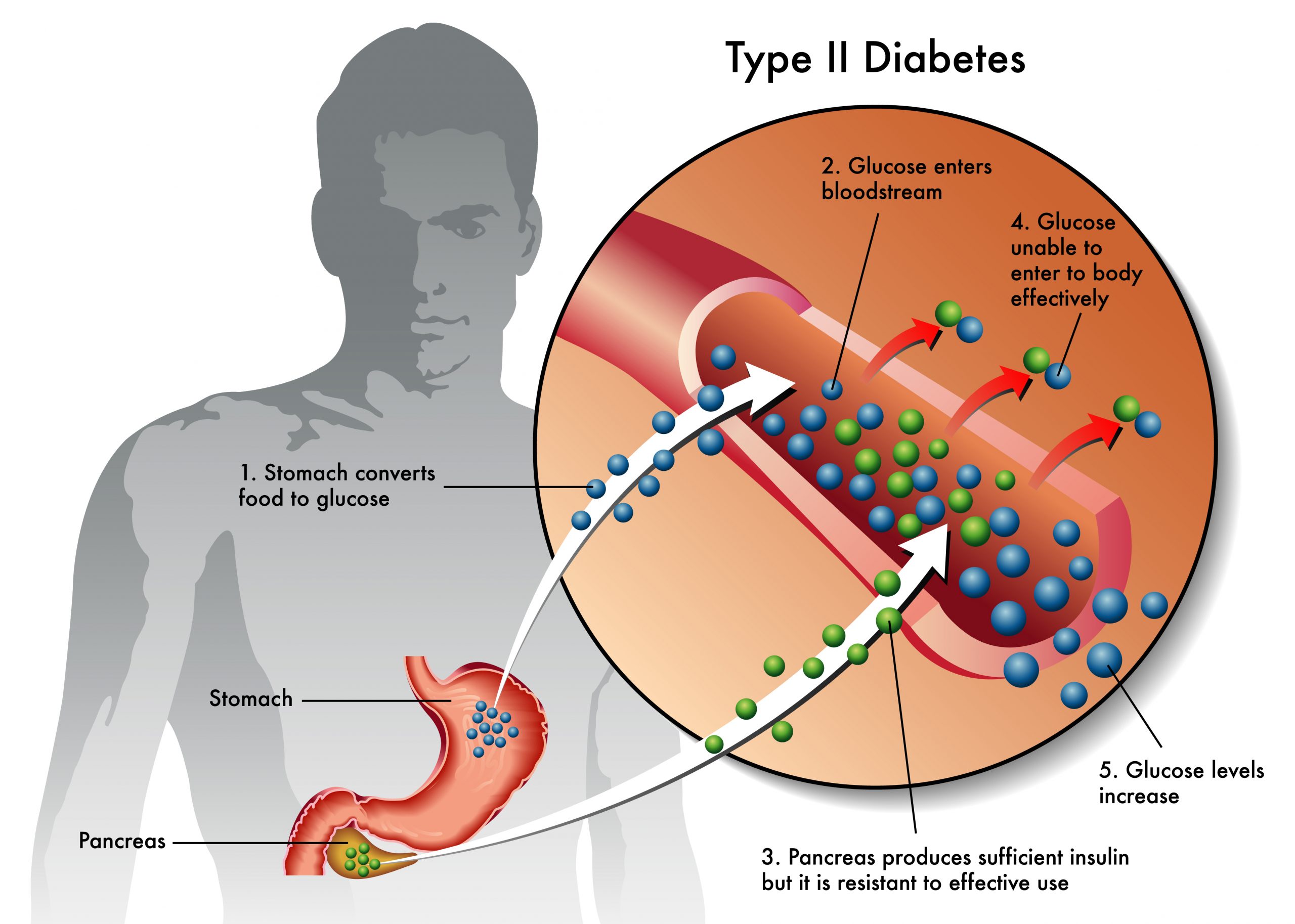
Insulin, Blood Sugar, and Type 2 Diabetes
- Insulin is a key player in developing type 2 diabetes. This vital hormone—you can’t survive without it—regulates blood sugar (glucose) in the body, a very complicated process. Here are the high points:
- The food you eat is broken down into blood sugar.
- Blood sugar enters your bloodstream, which signals the pancreas to release insulin.
- Insulin helps blood sugar enter the body’s cells so it can be used for energy.
- Insulin also signals the liver to store blood sugar for later use.
- Blood sugar enters cells, and levels in the bloodstream decrease, signaling insulin to decrease too.
- Lower insulin levels alert the liver to release stored blood sugar so energy is always available, even if you haven’t eaten for a while.
- That’s when everything works smoothly. But this finely tuned system can quickly get out of whack, as follows:
- A lot of blood sugar enters the bloodstream.
- The pancreas pumps out more insulin to get blood sugar into cells.
- Over time, cells stop responding to all that insulin—they’ve become insulin resistant.
- The pancreas keeps making more insulin to try to make cells respond.
- Eventually, the pancreas can’t keep up, and blood sugar keeps rising.
- Lots of blood sugar in the bloodstream is very damaging to the body and needs to be moved into cells as soon as possible. There’s lots of insulin, too, telling the liver and muscles to store blood sugar. When they’re full, the liver sends the excess blood sugar to fat cells to be stored as body fat. Yep, weight gain. And what’s more serious, the stage is set for prediabetes and type 2 diabetes.
NOTE: Type 1 diabetes is different; it’s thought to be caused by an autoimmune reaction (the body attacks itself by mistake). People with type 1 diabetes don’t make enough insulin and need to take it to survive.
Symptoms
(Type 2 diabetics)
- Urinate (pee) a lot, often at night
- Are very thirsty
- Lose weight without trying
- Always hungry
- Blurred vision
- Have numb or tingling hands or feet
- Fatigue
- Dry skin
- Slow healing sores or injuries
- Have more infections than usual
You’re at risk for type 2 diabetes if you:
- Have prediabetes.
- Are overweight.
- Are 45 years or older.
- Have a parent, brother, or sister with type 2 diabetes.
- Are physically active less than 3 times a week.
Treatment
Treatment consists of leading a healthy lifestyle, diet, and sometimes oral medications.
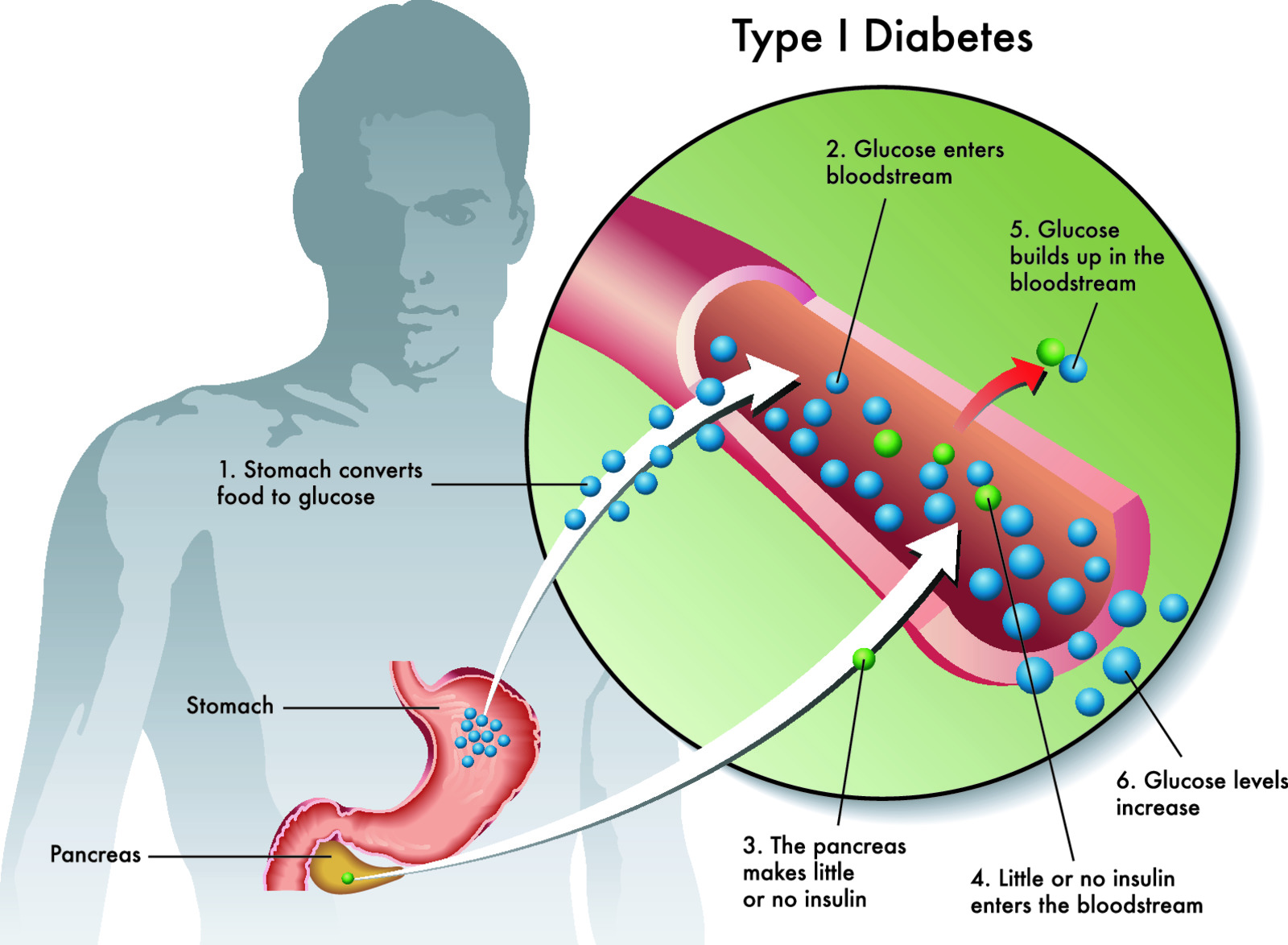
If you have type 1 diabetes, your pancreas doesn’t make insulin or makes very little insulin. Insulin helps blood sugar enter the cells in your body for use as energy. Without insulin, blood sugar can’t get into cells and builds up in the bloodstream. High blood sugar is damaging to the body and causes many of the symptoms and complications of diabetes.
Type 1 diabetes was once called insulin-dependent or juvenile diabetes. It usually develops in children, teens, and young adults, but it can happen at any age.
Only 5-10% of people with diabetes have type 1. Currently, no one knows how to prevent type 1 diabetes, but it can be treated successfully by:
- Following your doctor’s recommendations for living a healthy lifestyle.
- Managing your blood sugar.
- Getting regular health checkups.
- Getting diabetes self-management education and support.
Symptoms
In addition to the above symptoms listed for type 2 diabetes, type 1 diabetics may also have nausea, vomiting, or stomach pains. Type 1 diabetes symptoms can develop in just a few weeks or months and can be severe.
Treatment
Treatment consists of insulin therapy and sometimes oral medication in addition to leading a healthy lifestyle.
Gestational diabetes is a type of diabetes that can develop during pregnancy in women who don’t already have diabetes. Every year, 2% to 10% of pregnancies in the United States are affected by gestational diabetes. Managing gestational diabetes will help make sure you have a healthy pregnancy and a healthy baby.
What Causes Gestational Diabetes?
Gestational diabetes occurs when your body can’t make enough insulin during your pregnancy. Insulin is a hormone made by your pancreas that acts like a key to let blood sugar into the cells in your body for use as energy.
During pregnancy, your body makes more hormones and goes through other changes, such as weight gain. These changes cause your body’s cells to use insulin less effectively, a condition called insulin resistance. Insulin resistance increases your body’s need for insulin.
All pregnant women have some insulin resistance during late pregnancy. However, some women have insulin resistance even before they get pregnant. They start pregnancy with an increased need for insulin and are more likely to have gestational diabetes.
- Having gestational diabetes can increase your risk of high blood pressure during pregnancy. It can also increase your risk of having a large baby that needs to be delivered by cesarean section (C-section).
- If you have gestational diabetes, your baby is at higher risk of:
- Being very large (9 pounds or more), which can make delivery more difficult
- Being born early, which can cause breathing and other problems
- Having low blood sugar
- Developing type 2 diabetes later in life
- Your blood sugar levels will usually return to normal after your baby is born.
- About 50% of women with gestational diabetes go on to develop type 2 diabetes. You can lower your risk by reaching a healthy body weight after delivery.
Who is at risk
- Have ever had gestational diabetes (diabetes during pregnancy) or given birth to a baby who weighed over 9 pounds
- Overweight
- Over age of 25
- Not physically active
Symptoms
Unlike type 1 and 2 diabetes, there usually aren’t symptoms, it is usually diagnosed by urine and bloodwork.
Treatment
Depending on the severity of the diabetes, medication, lifestyle, and diet changes may be implemented.
- Brooke Lounsbury, RN
Medical Content Writer
Lifesaving Medications
Recent Posts
Keeping you informed and safe.
What Is Appropriate Medical Preparation? Meet the Medical Team Defining It
By Dr. Jamie Wilkey, PharmD — Director of Clinical Strategy, Jase American healthcare runs on a schedule. Monday through Friday, 8 to 5, in a well-populated area with decent coverage, it……mostly works. Expensive, slow, full of friction. But you can generally reach a...
The War Nobody Prepared For: How the Iran Conflict Is Threatening Your Medicine Cabinet
*By the Jase Medical Clinical team* Most Americans think of war as something that happens somewhere else, visible mainly through a screen. The Iran conflict has found its way into something far more intimate: the medicine bottles in your bathroom cabinet.Since Iran...
Your Immune System Can Fight Cancer
*By the Jase Medical Clinical team* For decades, the dream in oncology has been simple and audacious: teach your own immune system to hunt cancer. Not poison it with chemotherapy. Not burn it with radiation. Train your body's existing defenses to do what they were...